WHAT IS THE SIGNIFICANCE OF DELAYED DENTAL TREATMENT IN THE GENERAL HEALTH OF OUR PATIENTS?
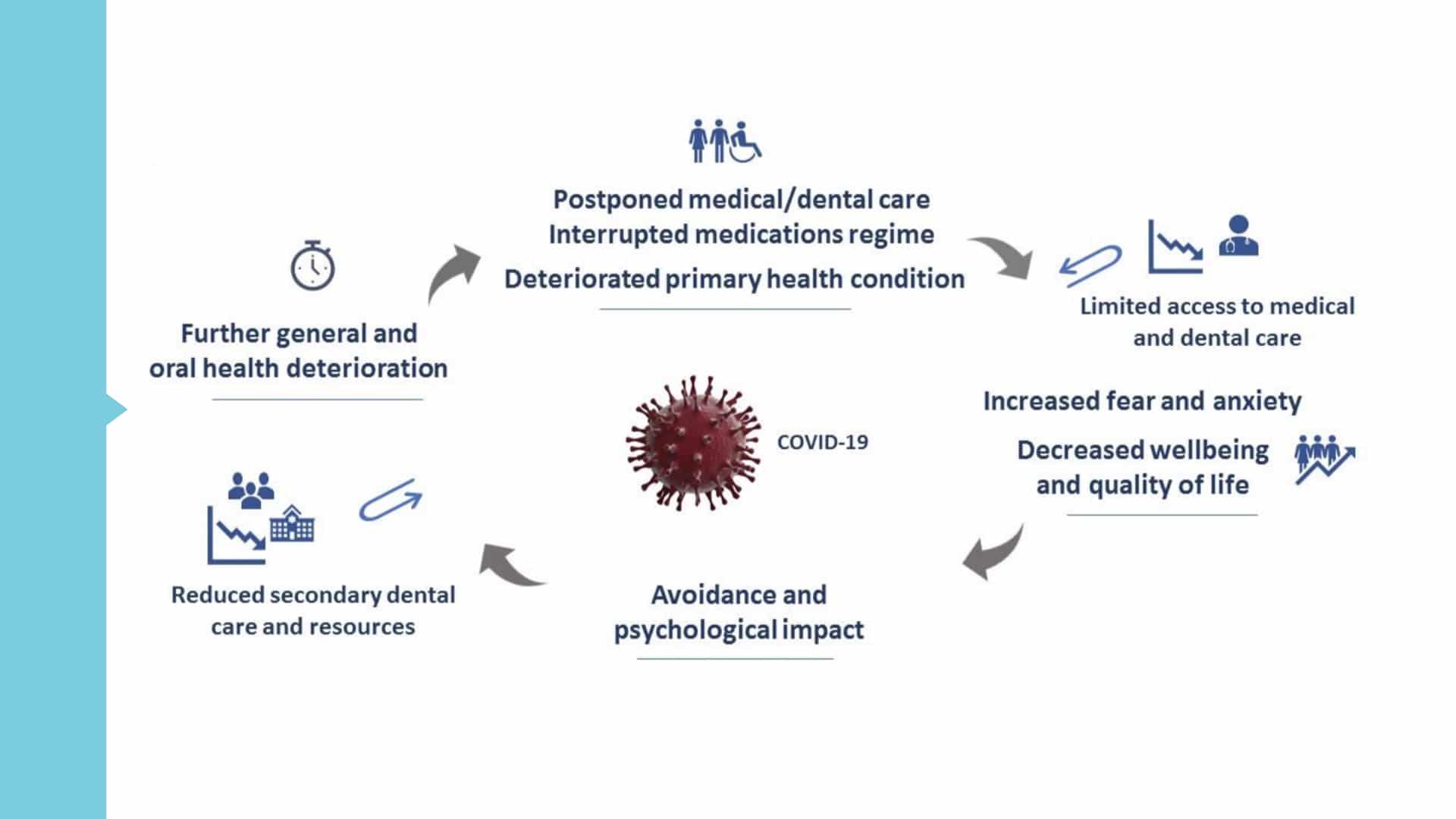
CoVid-19 pandemic has affected our way of life especially the way we have to do our dental practice. We are constantly in fear and in paranoia to contract this virus every time we practice our profession to the point that others still have not opened their dental clinics or have retired or even sold their dental business. For those who are still practicing, there are so many requirements and steps to do just to make sure we protect ourselves and our staff and one of those steps applied by others is delaying dental treatments unless it’s critical or emergency cases. Thus, this step may produced a compounding negative result to our patients’ total general health at a later date.
Recently, I attended a webinar of PSP that discusses oral health in relation to CoVid-19 and it provided interesting information that inspired me to write this topic. I ended up musing what’s happening now and what will be the effect of our actions now as dental professionals into the future such as the delegation of oral health being secondary and its seemingly disconnect of its significance to the over-all health; the effect of our delayed treatment to our patients when it is not an emergency or critical case; the main reason that drives our dental practice in this new norm and our moral dilemma as dental practitioners.
ORAL DISEASES AND ITS RELATION TO GENERAL HEALTH
There are already several research and studies that links oral conditions to general health. In fact, there are a lot of diseases that its signs and symptoms are manifested in the mouth first. In oral conditions, periodontitis seems to show the leading cause that may create damage elsewhere in the body. There are several studies that supports its contribution to several health issues such as cardiovascular disease, diabetes, respiratory conditions, Alzheimer’s disease, pre-term birth, cancer, etc. This theory of focal infection has high significance now more than ever in the light of CoVid-19 pandemic as many recent review studies and evidences in several randomized clinical trials show that periodontitis demonstrates to have a negative impact on respiratory conditions and lung function with CoVid-19 infected patients. They all point to the importance of the connection between oral bacteria and the respiratory tract.
In the studies from the Journal of the California Dental Association in October 2020, it has been established that untreated periodontitis causes inflammation and increases pro-inflammatory cytokines such as IL-6 in the general circulation. It also established the fact that IL-6 has been considered as a critical predictor for respiratory complications in COVID-19. It is therefore their conclusion that periodontitis can increase the risk of respiratory complications in COVID-19 patients. This is also greatly apparent in the studies done in Germany and Japan which reflects the importance of dental plaque and oral hygiene in COVID-19 infected patients. As mentioned in the webinar, a recent study in Japan shows hospitalized COVID-19 patients provided remarkable information to confirm the importance of dental plaque for virus shedding. The researchers followed eight COVID-19 patients who were over the acute symptomatic phase, but remained positive to SARS-CoV-2. On this clinical research, the virus was still detected on the patients despite recovery after 15.1 days on average. However, two patients remained positive for the virus for 44 and 53 days. Those two patients were not performing daily oral hygiene due to mental and/or psychiatric disorders, and they were instructed to start toothbrushing and use mouthwash with help from nurses. Four to nine days after oral hygiene was initiated, both patients tested negative.
These studies clearly show why local infection and inflammation in the mouth can affect the rest of the body, including the entrance of oral bacteria and/or their toxic products into the systemic circulation, systemic inflammation, endothelial dysfunction, gut dysbiosis, and local lung changes. And, even if you are just practicing general dentistry it is obvious that the mouth is not separate from the body and that oral bacteria can have negative effects on other organs, thus, delaying dental treatment underestimates the interconnection and correlation between mouth and body.
FEAR CONTROLLING OUR PRACTICE
As dental practitioners we are bound to our duty to treat our patients, but, this pandemic created much fear in all of us that we are place between a rock and a hard place. This is not simply just protecting ourselves but also our love ones if we become infected and a carrier. In the presence of some being asymptomatic but a carrier, fear became a major emotion as we do our dental practice. This is only natural otherwise we are not human, so, basing our decisions on a comprehensive study and irrefutable conclusive truths and facts about this virus becomes secondary as we start to practice on a defensive mode first of what we just know now.
Even before CoVid-19, we should be practicing high standard of infection control due to possible patients who are potential carrier of contagious diseases, such as hepatitis and HIV. The way we do our infection control in our dental practice should have been the normal standard and not the “new norm” to decrease occupational health issues and cross-infection among the dental community. Thus, starting on this premise, the main issue now is dealing with our fear. One of the things that generates our fear is handling the aerosols and droplets which have been pointed out as a potential culprit in the context of COVID-19 spread. However, let it be known that no current studies show that dental-generated aerosols have viable viral particles. Only studies using viral culture can provide data on the infectivity of dental aerosols, as PCR tests can confirm the presence of minute amounts of viral RNA, but cannot necessarily confirm the presence of infectious viruses. There are also studies now that show dental aerosols are different from medical aerosols because they result mainly from water irrigation, having the potential to dilute viral particles. Besides, the high-volume evacuation systems used in dentistry significantly decrease aerosols situation. Hence, what’s the fear? Fear is greatly generated by the unknown and as stated in the “Natural history of asymptomatic SARS-CoV-2 infection” published in N Engl J Med. 2020, “typically, the greater the imminent threat to public health, the lower the standards of evidence in early guidance. So, there are still several questions that needs to be addressed in order to develop and refine future guidance for infection control in the dental setting.”
This means as we go about our dental practice, we have to be very cautious but we shouldn’t allow our fear to run amok the way we do our dental practice. We have to arm ourselves with evidence-based knowledge and continually study about this virus, so, we can base our decisions in our practice on irrefutable facts rather than our unsubstantiated fear.
OUR MORAL DILEMMA
As dental practitioners in the new norm due to this pandemic, it raises the issue of moral versus evidence-based decisions. Personally, “evidence-based” is one of the terms being used in our practice that I have a love-hate relationship with not because I don’t believed in it but how this term is being often used to manipulate and control the way we need to learn. Having said that, on this pandemic, this term needs to come into play. Why? Because precisely this a very good tool so we can weigh our decisions properly especially when we are morally bound to do something that we don’t want to do.
In the practice of dentistry, it is very hard to treat patients without personally seeing the patient. It is simply a given fact, however, recently, we are forced to do digital ways to address our patients’ concerns such as teledentistry. It is very important to consider that most patients who have periodontal disease present no obvious pain, thus, it is very easy to be ignored or missed as we go about our initial consultation with our patients through teledentistry, despite that this condition can be the hidden source for chronic infection and inflammation. The effect of establishing prevention and treatment of oral diseases now can have a positive impact on COVID-19 directly and indirectly. Directly because it can reduce local and consequently general inflammation, and indirectly because it decreases the risk for other conditions that are linked to higher COVID-19 mortality, such as cardiovascular disease and diabetes.
Unfortunately, we have to take certain steps that maybe difficult for us to properly treat our patients but these steps need to be done as of the moment as we are all still continually learning about the exact nature of CoVid-19. However, it must be point out and said that currently there are still a lot of multiple missing links about the transmissibility of SARS-CoV-2 in dental clinics, particularly in aerosols. Also, there has been no data to suggest higher infection rates among dentists and dental staff and higher risk for patients to become infected as a result of dental treatment. But, in the ere of caution, WHO’s moral decision to delay non-essential dental interventions became relevant at the start of this pandemic due to the urgency to protect health professionals and patients. Knowing what we know then and what we know now which shows that this pandemic seems here to stay and become our reality, WHO’s decision to only address emergency cases or critical ones as much as possible has become unsubstantiated because delaying treatment of oral conditions can also deteriorate the general health of our patients. This realization is greatly felt by majority of dental professionals all over the world and as ADA President Chad P. Gehani stated, “Oral health cannot be ignored as it constitutes an integral part of overall health. Thus, essential healthcare cannot be complete without dentistry.”
CONCLUSION
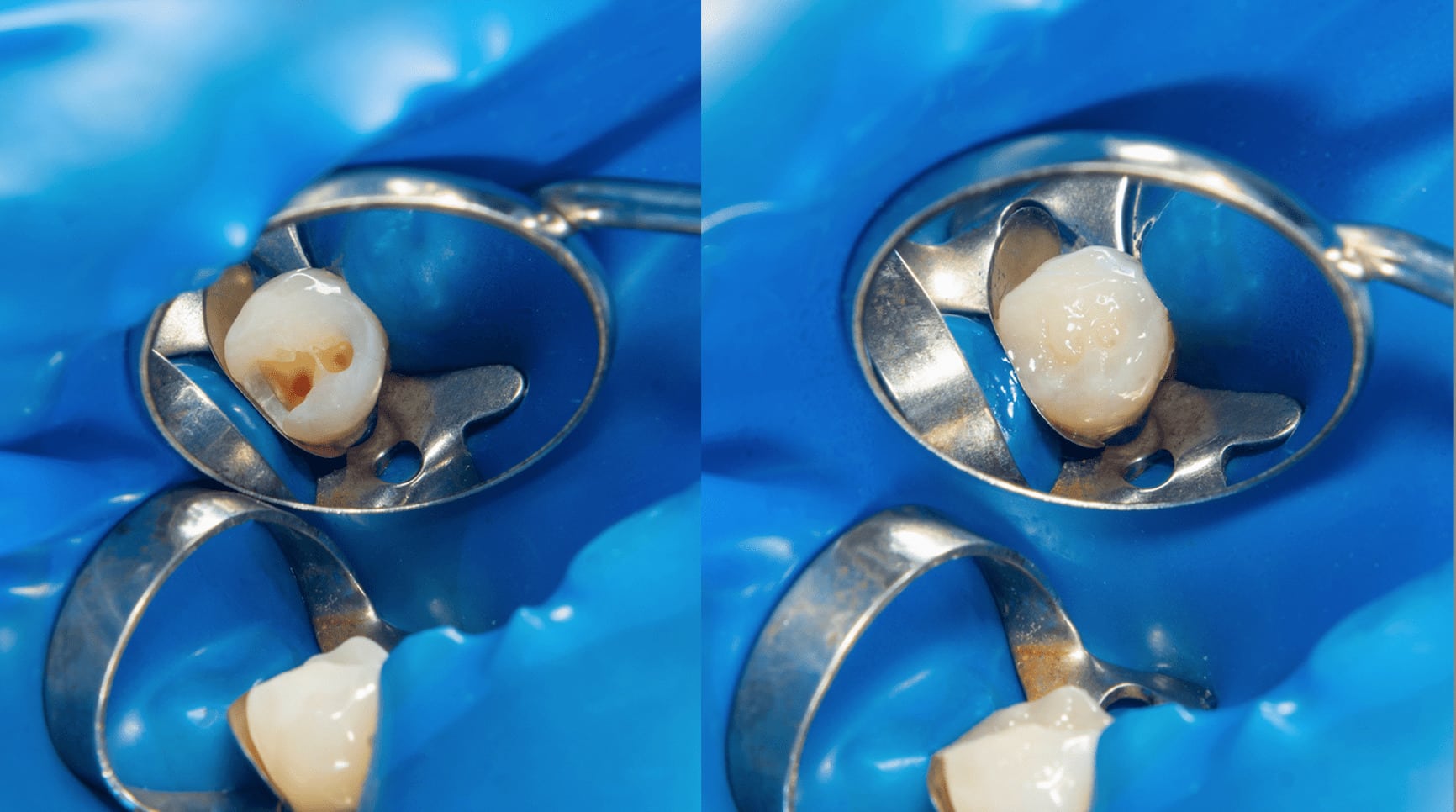
In a situation like this, we as health providers know fully well that our role as dentists through our dedication and commitment are indispensable healthcare providers during these challenging times and for those who continually do their dental practice and do such great work deserve to be fully recognized and supported by all health organizations, given the importance of oral health for general health and well-being. As health givers we are bound to do as much as we can to relieve and be an integral part of maintaining the health of the public during this difficult times. It is very significant to take into consideration that we cannot forever delay what we need to do as dentists and treat our patients no matter how non-critical the dental case maybe just like doing oral prophylaxis as this may, in the end, have a far-reaching effect in the long run on their general health.
For further information on this regard in relation to Oral Health and CoVid-19, you may download here the article : CLICK HERE: [Download not found] entitled: "The Mouth-COVID Connection: Il-6 Levels in Periodontal Disease — Potential Role in COVID-19-Related Respiratory Complications by: Shervin Molayem, DDS, and Carla Cruvinel Pontes, DDS, MsC, PhD.
CONTRIBUTOR
Dr. M. Jean Villanueva - Editor | Writer
REFERENCES
1. Sakurai | A Sasaki T | Kato S et al. Natural history of asymptomatic SARS-CoV-2 infection. N Engl J Med. 2020; (published online June 12.) https://doi.org/10.1056/nejmc2013020
2. Dr. Molayem DDS at the UCLA School of Dentistry. Dentistry Today
3. US CDC Guidance for dental settings. Interim infection prevention and control guidance for dental settings during the COVID-19 response. https://www.cdc.gov/coronavirus/2019-ncov/hcp/dental-settings.html Date accessed: July 30, 2020