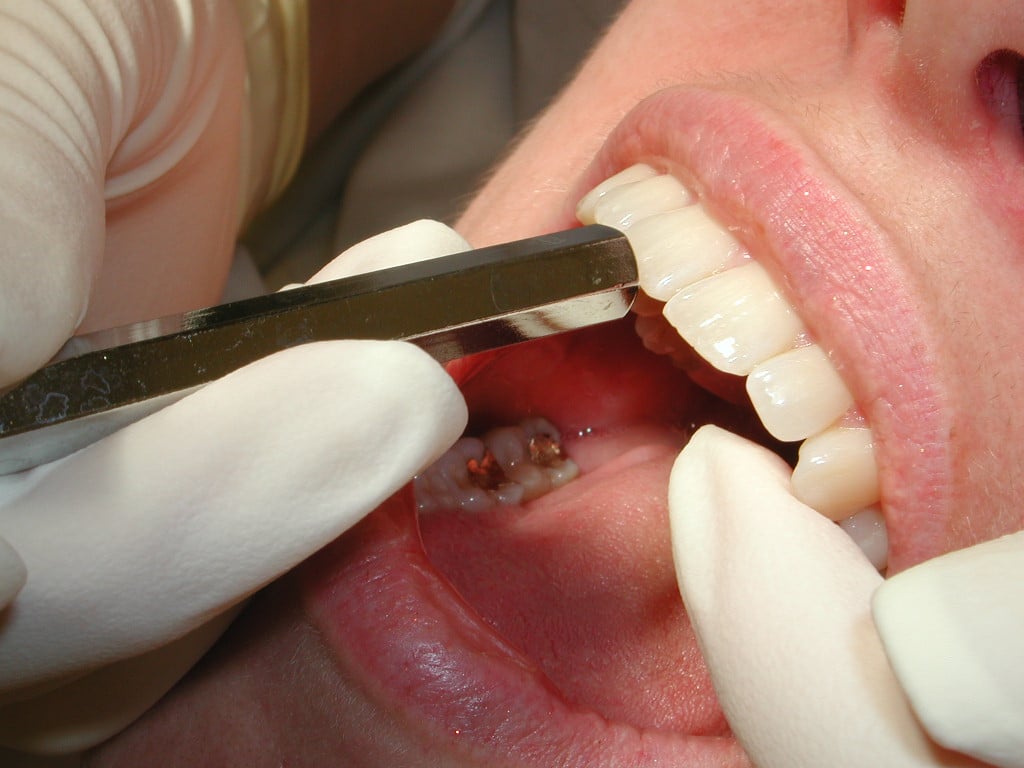
Is The Application of SILVER Diamine Fluoride (SDF) the answer to Caries Prevention In children & Young Adults?
The high prevalence of caries among children and young adults has already been a concern for a long time among the dental community globally and in our country especially on various dental Pediatric organization. Base on the study done published on 2005, "Prevalence of dental caries and sugar consumption among 6–12 year old schoolchildren in La Trinidad, Benguet, Philippines", its data shows that there's 68.2% prevalence of dental caries in primary and permanent dentition, respectively, among schoolchildren aged 6–12 year old in La Trinidad, Benguet, Philippines, indicating a widespread neglect of oral health in the children. Untreated decayed teeth dominated the DMFT (Decayed | Missing | Filled Teeth) scoring among the children demonstrating a high rate of unmet treatment needs. It substantiates the Philippines National Oral Health Survey Report, which described high caries prevalence rates in the permanent dentition of 12-y-old children (Department of Health, 1998). It has further described that there's so many children who haven't even seen a dentist for a check-up. And, the statistics shown that there’s only little improvement through the years on this situation since its publication. Thus, the Philippine Pediatric Dental Society, Inc. (PPDSI), currently led by Dr. Paul Abaya, made its mission with the project, "Bata Muna" to address precisely and improve this condition.
With this current situation, it is now important that as dentists even if Pediatric Dentistry is not our primary specialty of practice, we need to share the responsibility of supporting this endeavour and learn more about treatment options that we can safely use to our patients whether children or adults to be part of lowering down caries incidence in our own society or community.
One of the treatment options to prevent or arrest caries is the application of Silver Diamine Fluoride (SDF). Thus, this post will try to provide as much as we can to provide initial awareness and information about this treatment, so, as a dental professionals one can delve deeper more into it by attending webinars or doing further research if this SDF can truly at the end of the day help in arresting caries of our patients especially for children and young adults.
ABOUT SILVER DIAMINE FLUORIDE
Silver Diamine Fluoride (SDF- 38% w/v Ag(NH3)2F, 30% w/w) is a clear, odourless liquid applied topically comprised of 24.4-28.8% (w/v) silver and 5.0-5.9% fluoride, at pH 10,4 and marketed as Advantage Arrest by Elevate Oral Care, LLC (West Palm Beach, FL). It is indicated for desensitisation of non-carious tooth lesions and molar incisor hypomineralisation. It considered as an inexpensive topical medicament used extensively in other countries to treat dental caries across the age spectrum since its approval in Japan over 80 years ago. By far, since its release more than two million containers have been sold in the dental market. The silver content acts as an antimicrobial, the fluoride promotes remineralization, and the ammonia stabilizes high concentrations in solution. No other intervention approaches the ease of application and efficacy.
SILVERM DIAMINE FLUORIDE FUNCTION
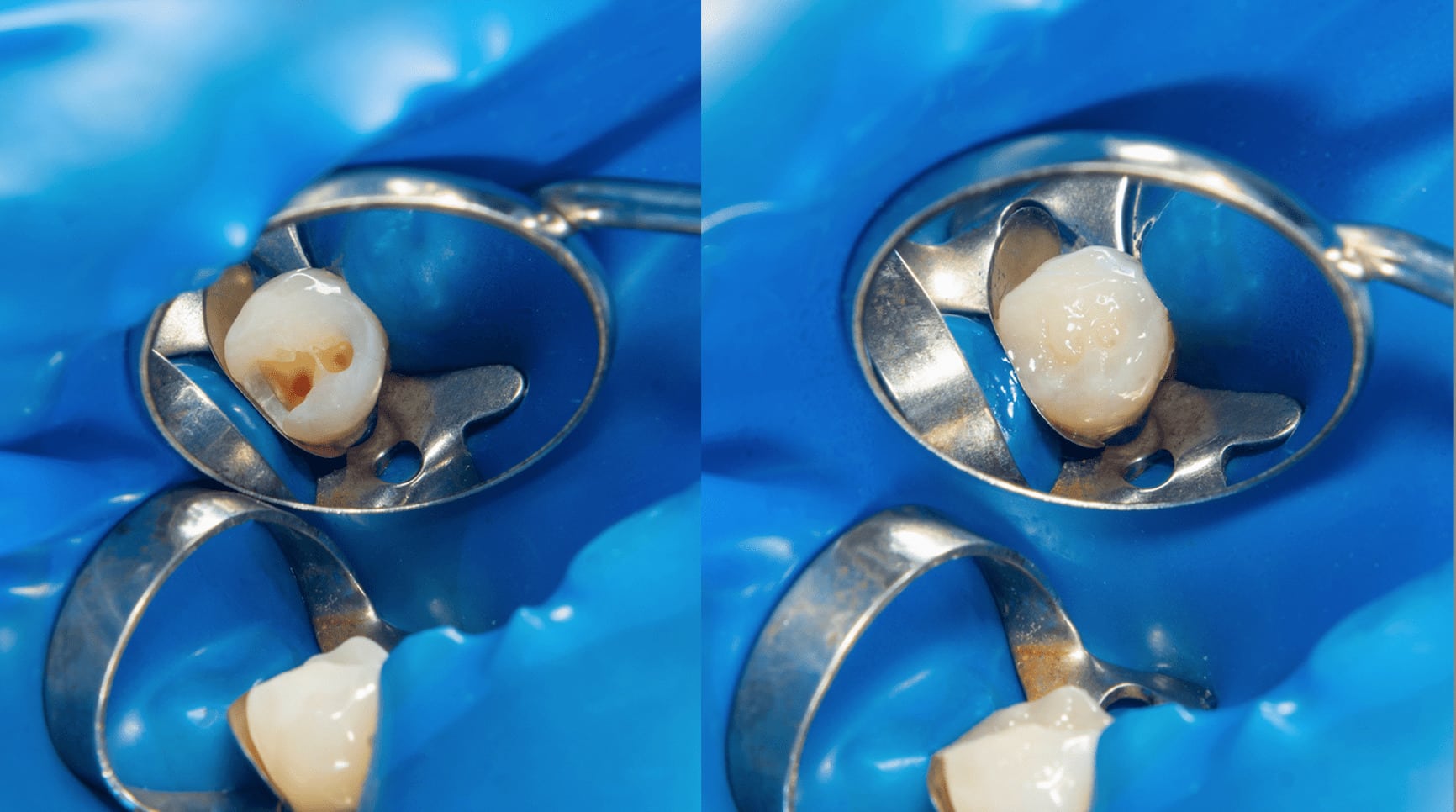
- To arrest and slow the rate of caries progression.
- Treatment of dentin hypersensitivity.
SILVER DIAMINE FLUORIDE APPLICATION
- Brush On
- Dab with Cotton Swab
SILVER DIAMINE FLUORIDE STEPS
- Dispense SDF into a dapper dish.
- One drop treats five surfaces.
- Isolation with gauze and/or cotton rolls is sufficient. And, air-drying prior to application improves its effectiveness.
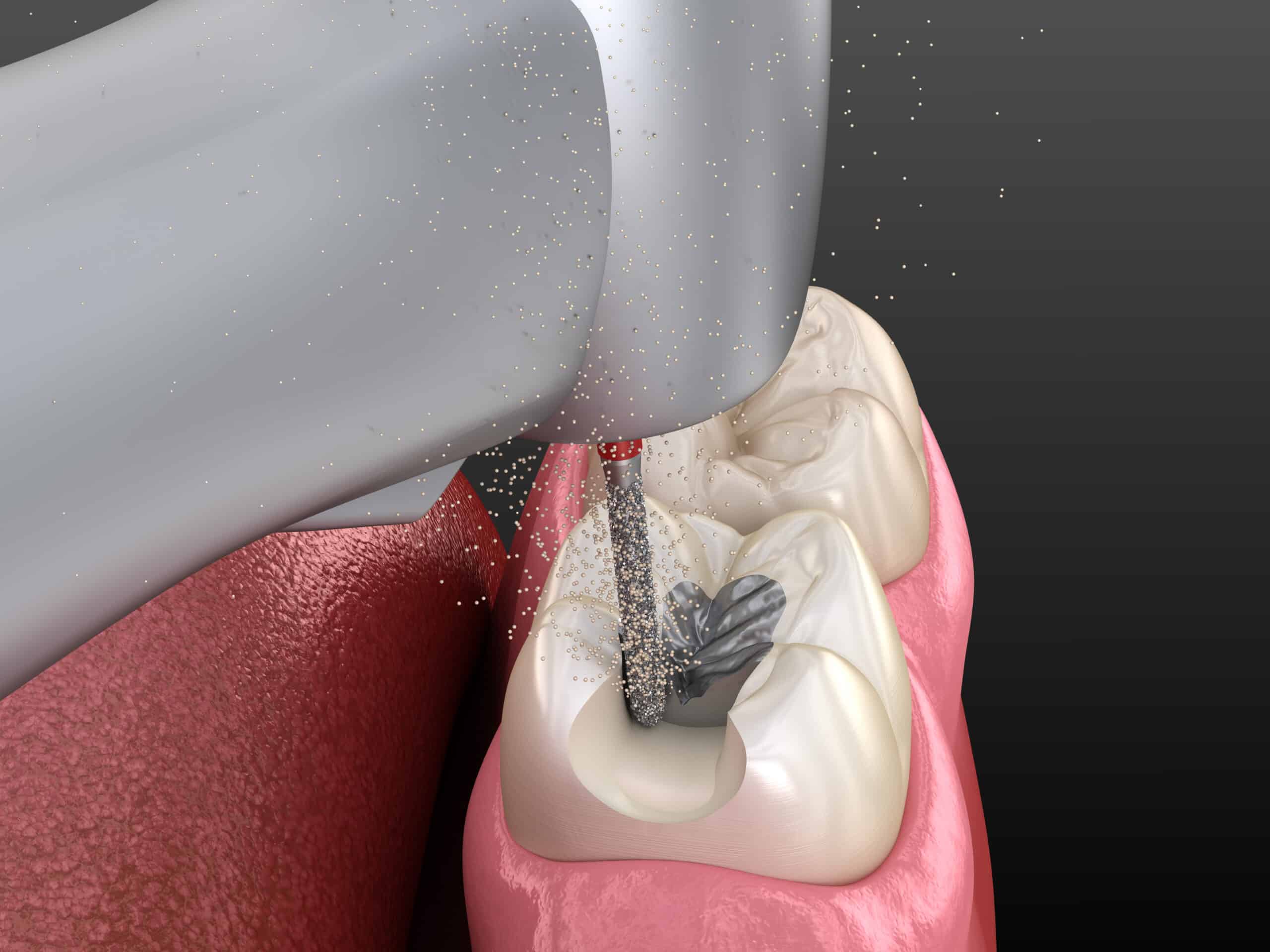
- Immerse a stiff micro-brush into the SDF in the dapper dish and saturate the lesion with SDF using a scrubbing motion.
- Allow 1-3 minutes for the silver diamine fluoride to soak into and react with the lesion to make it effective.
SILVER DIAMINE FLUORIDE MODE OF ACTION
- Inhibits demineralisation of tooth enamel.
- SDF Mechanism Upon application of silver diamine fluoride to a decayed surface, the squamous layer of silver-protein conjugates forms, increasing resistance to acid dissolution and enzymatic digestion.
- Silver ions act directly against bacteria in lesions by breaking membranes, denaturing proteins, and inhibiting DNA replication. Ionic silver deactivates nearly any macromolecule.
- Silver diamine fluoride outperforms other anti-caries medicaments in killing cariogenic bacteria in dentinal tubules.
- Promotes remineralisation of tooth mineral, hydroxyapatite.
- Hydroxyapatite and fluoroapatite form on the exposed organic matrix, along with the presence of silver chloride and metallic silver. The treated lesion increases in mineral density and hardness while the lesion depth decreases.
- Silver and fluoride ions penetrate ~25 microns into enamel, and 50-200 microns into dentin.
- Fluoride promotes remineralization, and silver is available for antimicrobial action upon release by re-acidification.
- Silver diamine fluoride arrested lesions are 150 microns thick.
- Address Dentin Hypersensitivity
-
In treatment of exposed sensitive dentin surfaces, topical application results in development of a squamous layer on the exposed dentin, partially plugging the dentinal tubules. High concentration aqueous silver has been long known to form this protective layer. Decreased sensitivity in treated patients is consistent with the hydrodynamic theory of dentin hypersensitivity.
SILVER DIAMINE AND BONDING
Effects on bonding with the use of current bonding system, the silver diamine fluoride had no effect on composite bonding to non-carious dentin with the use of either self-etch or full etch systems. There’s one study that states with simply rinsing after silver diamine fluoride application avoids a 50% decrease in bond strength for GIC. While in another study, there’s an observation of increase of dentin bond strength to GIC. However, Silver Diamine Fluoride may decrease dentin bonding strength of resin-based crown cement by ~1/3. Thus, rinsing for direct restorations maybe needed, while excavation of the silver diamine fluoride-treated on superficial dentin is appropriate for cementing crowns.
SILVER DIAMINE ADVANTAGES
- Relatively Inexpensive
- Easy to Apply
- Non-Invasive
- Requires Minimal Training
- Slows and Halts Disease Progression
SILVER DIAMINE DISADVANTAGES
- Black Staining
- Components of Silver and Fluoride
- Fluorosis
REFERENCE ON FLUORIDE
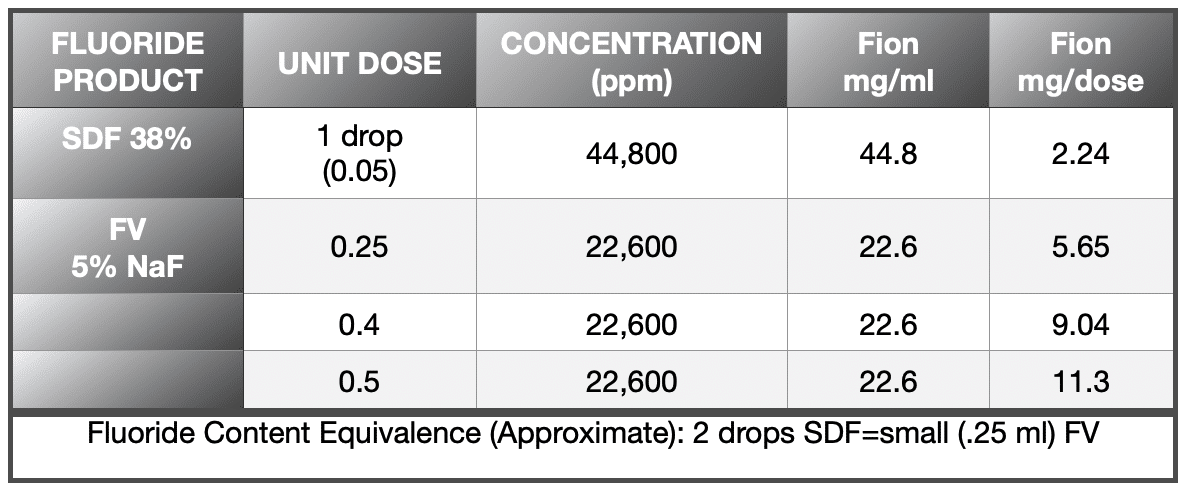
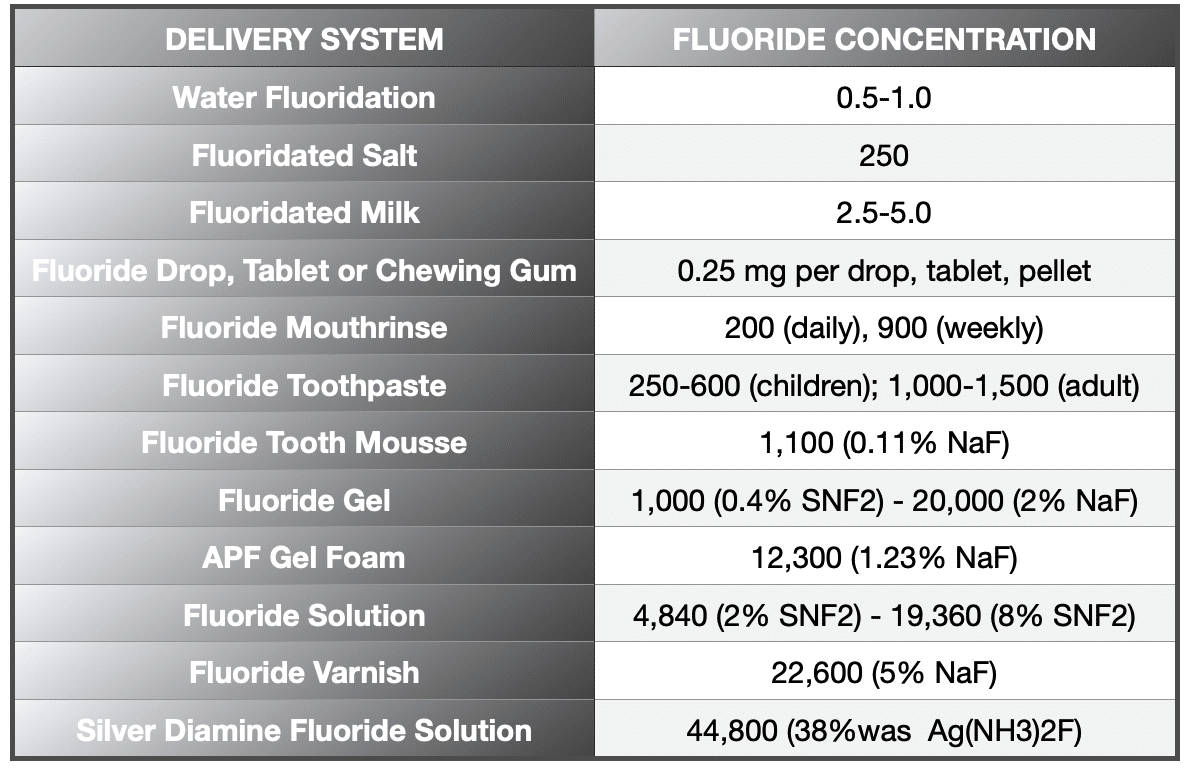
CONCLUSION
There’s no treatment that fits all situations. However, base on the studies I’ve read this treatment is FDA cleared for dentinal hypersensitivity that’s similar to fluoride varnishes’ function. This can be used for adults over the age of 21 and, effective in increasing dentinal hardness and provides a painless treatment for blocking dentinal tubules to address its sensitivity. It is also important to take note that this treatment has been used for more than 50 years in Japan, China, India, New Zealand, Australia and many other countries as a caries arresting agent. And, through its years of use, there’s no severe health risk or adverse effects have been reported. However, it is contraindicated for patients known with silver allergy.
Whether this treatment is indeed a great tool to address the prevailing increase of caries incidence in our country and globally seems to be, in my humble opinion, something to be considered especially its application is very doable particularly in remote areas that decent dental clinics are hard to come by and its disadvantages outweighs its benefits in the long run especially for temporary and posterior teeth of children and young adults.
CONTRIBUTORS:
Dr. Jean Galindez – Editor | Writer
REFERENCES:
1. Silver Diamine Fluoride (SDF) Treatment And Outcomes by Tristan Galloway, DDS
2. Silver Diamine Fluoride. Presented by Diana Pham, Dental Hygiene Student Kimberly Truong, Dental Hygiene Student Lamar Institute of Technology Dental Hygiene Program. Silver Diamine Fluoride “The Silver Bullet”. Importance to the Hygienist 2 components: Silver and Fluoride
3. The use of silver diamine fluoride (SDF) in dental practice. Nassar Seifo, Mark Robertson, Jeanette MacLean, Katharine Blain, Sarah Grosse, Roderick Milne, Clement Seeballuck & Nicola Innes British Dental Journal volume 228, pages75–81(2020)