What Are the Risk and How to Manage Odontectomy?
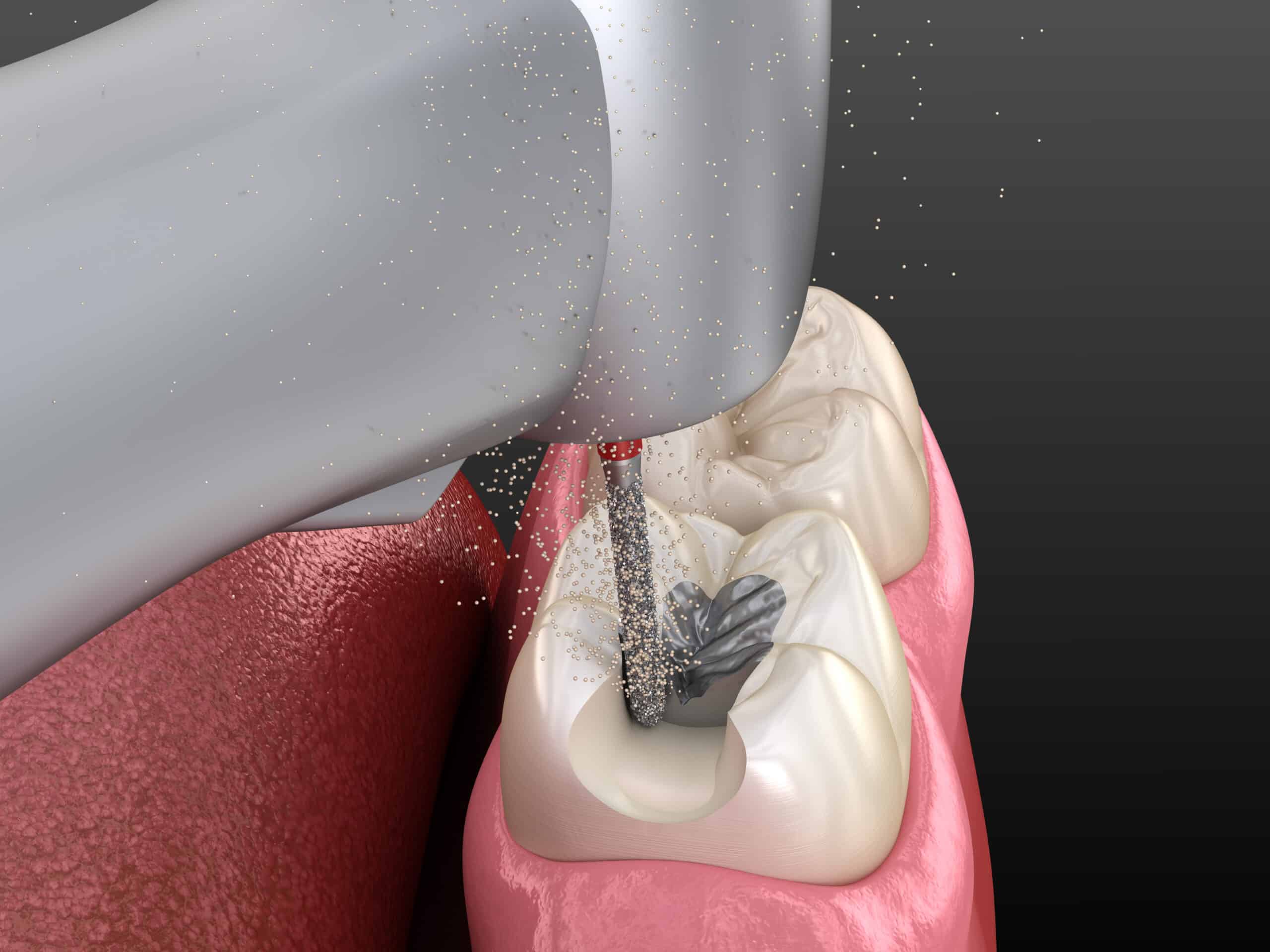
Odontontectomy or Third Molar surgery is one of the most common procedure performed by dentists and oral maxillofacial surgeons in clinical practice. This procedure requires accurate planning and execution. Generally, this procedure is quite predictable, so, possible complications can be infrequent. Nevertheless, we should still know these complications and how we should manage them in case it happens.
This post is to review the presentation and management of the common complications associated with odontectomy, with emphasis on avoidance and management of the procedure. This acts as a review for the general dental practitioners, as well as the oral and maxillofacial surgeons, that it is still important to be familiar with all the possible complications. This will improve on how we can properly provide our patient's education on the treatment they will go through for better management on pre and post steps that's needed for a successful treatment.
PARESTHESIA
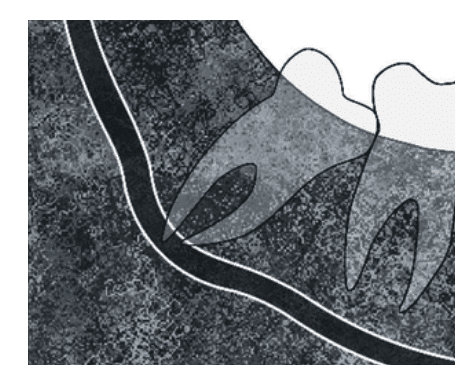
The most common cause of malpractice related to odontectomy is paresthesia of the lip or the tongue. It is imperative to take through planning and workup in preventing this complication. Radiographic signs on a panoramic xray such as darkening of the root in area of the mandibular canal(A) , diversion of the mandibular canal (B) or an interruption of the radiopaque border of the mandibular canal (C) may be indicator of increased paresthesia risk.
FIGURE A
FIGURE B
FIGURE C
Lingual paresthesia is worst for the patient than lip paresthesia. It often occurs when the operator improperly places the incision too far to the lingual aspect of the alveolar ridge. It can also occur from excessive retraction of a lingual flap, or during tooth sectioning that is carried too deeply. Clinicians should bear in mind that distal to the third molar, the lingual nerve may take a course that is very high in the alveolus. CBCT is proven helpful in identifying the location of the IAN.
If paresthesia that is not improving within a three-month period or more than the usual healing period, it should be referred for consultation to an oral and maxillofacial surgeon or a pain management specialist (the consultation should at least be suggested to the patient) because the success of nerve repair is greatly affected with timely intervention.
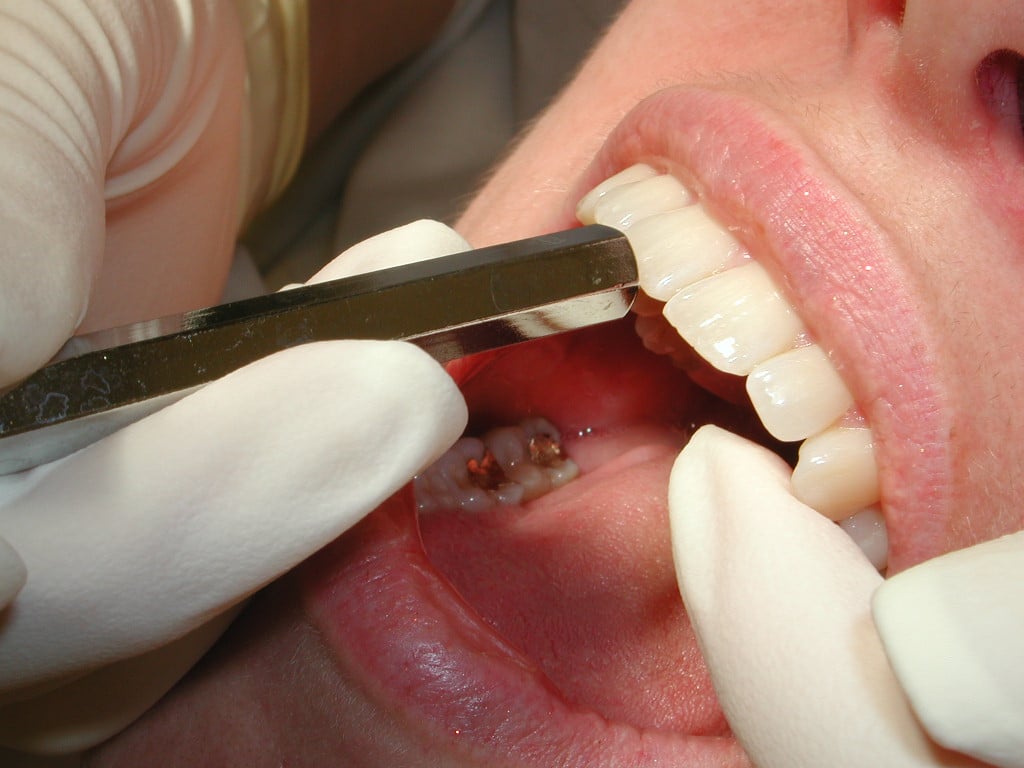
EXTRACTION OF THE WRONG TOOTH
This complication is largely avoidable, yet it remains a common cause of malpractice claims. There are cases that the 2nd molar is extracted instead of the distally positioned 3rd molar. The key in prevention is communication between parties involved. The staff should also be empowered to call out if they see any error about to happen or during its procedure. Moreover, counter checking helps by marking the tooth in the radiograph which can greatly lower the chances of committing this kind of errors.
If the wrong tooth is extracted, the oral surgeon should proceed with removing the correct tooth unless the extraction is for orthodontic purpose. It may be better to seek the advice of the patient's orthodontist first.
If the tooth extracted by mistake is otherwise healthy, it should be immediately replanted on its socket. If mobile, it should be held in place with a custom made vacuum-formed splint for approximately 4 weeks. If there is any doubt about its prognosis, take a radiograph and assess if the tooth will require RCT later on.
SUBCUTANEOUS EMPHYSEMA
Subcutaneos Emphysema occurs when air emitted from a turbine-driven handpiece is forced into a surgical space. It generally presents with sudden facial swelling and soft tissue crepitus.
Antibiotics are indicated to prevent infection. While usually self-limiting, there are numerous cases reported that have resulted in severe mediastinal infection, or an embolus traveling to the heart. Thus, it is imperative that any open surgical procedure in the oral cavity be performed with a reverse-air handpiece, rather than a standard handpiece that could force air into a wound.
TISSUE DEHISCENCE
Wound dehiscence is defined as a partial or total separation of previously approximated wound edges, due to a failure of proper wound healing. Wound dehiscence include soft tissue trauma, improper flap design, excessive tension on a flap, infection, or a compromised health of the host. Generally, there is no specific treatment other than good oral hygiene and allowing the wound to heal by secondary intention. Attempts to re-close the wound are usually unsuccessful.
During creating a flap, the operator should keep in mind that the incision should not be performed on bone defects, or cut the muscle or tendon, the incisions should not be very long as this may result to the unfortunate consequences of wound dehiscence.
It is suggested to do an envelope flap with a distal releasing incision or a triangular flap as a common approach for lower third molar surgery and mesioangular impaction is the most prevalent type of impaction in the lower jaw.
ALVEOLAR OSTEOTITIS (DRY SOCKET)
The most common complication in surgery is dry socket. The condition is most common with mandibular third molars and more common in females (especially if on oral contraceptives). Smoking, surgical trauma, food impaction and lengthy procedure cause the patient a patient to dry socket. Occurring three to five days postoperatively, dry socket presents as a dull and aching pain which can radiate up to the ear if left untreated.
Patients will often say that it “feels like a toothache.” Examination of the site will reveal complete absence of a blood clot or necrotic-looking, incomplete clot formation. There may be a fetid odor. It is important to rule out infection, so there should be an absence of fever, increasing edema or purulent drainage.
Alveolar osteitis is treated by irrigating the socket with saline and placing an anodyne (sedative) dressing. Analgesics are usually indicated, and the patient should be followed in 48 hours. Repeated treatments may be needed until the patient is comfortable without a dressing.
In terms of prevention, clean, efficient surgical technique with bone-cooling irrigation during drilling is critical. There is also evidence that pre- and postoperative chlorhexidine rinses and chlorhexidine gel placed into the socket will reduce the incidence of dry socket.
DISPLACED ROOT FRAGMENTS
Accidental displacement of impacted third molars, either a root fragment, the crown, or the entire tooth, is not common during extraction, but is a well-recognized complication.
Roots or root fragments can be accidentally displaced into the sinus, mandibular canal, sublingual and submandibular space, or the infratemporal fossa. The best way to prevent this is to avoid excessive force directed in a vertical direction when the root lies in direct contact with the sinuses. A thorough understanding of the radiograph is also required to properly plan your approach on this kind of cases.
Attempting to retrieve the root from the maxillary sinus or mandibular canal or deeper fascial spaces is not recommended if you are not well-trained to do this procedure just so to avoid further complications. Generally, it is wise if you refer the case and have it managed by an experienced oral and maxillofacial surgeon.
BONE FRACTURE
Fractures of the mandible or of the maxillary tuberosity have been known to occur in association with wisdom tooth extraction. Fractures may occur with improper instrumentation and excessive force placed on the bone during tooth removal.
The reduction of bone strength may be caused by physiologic atrophy, osteoporosis, pathologic processes, or can be secondary to surgical intervention .
Due to the higher level of masticatory force, men may be more likely to have late fractures. Most late fractures occur between two to four weeks after surgery during masticating.
When you experience a fracture during odontectomy, we recommend that you stop doing the procedure. Then, one should stabilize the jaw with a cloth or hand, prescribe the necessary meds like Arcoxia and take a CBCT. Finally, refer the case to a specialist as soon as possible. DMD Center created a post regarding referrals, you may CLICK this to READ THE POST.
TEMPOROMANDIBULAR JOINT TRAUMA | TRISMUS
A certain amount of trismus secondary to trauma and inflammation of the adjacent muscles of mastication sometimes occurs as a result of wisdom tooth extractions. Improper instrumentation, hyperextension of the jaw may also cause trismus. This occurs when a needle delivering the anesthetic solution inadvertently damages surrounding tissue. If a patient has preexisting TMJ pain, it is important to document this dental history pre-operatively. Delayed-onset trismus generally involves possible presence of infection. Another thing, it is important to take note that persistent joint pain may require additional workup to rule out any other joint disorder.
Moist heat and anti-inflammatory medications will be helpful in management. Perioperative and postoperative steroids or nonsteroidal anti-inflammatory drugs have been shown to reduce edema and trismus following third molar surgery. In addition, the use of a bite block is advisable to minimize trauma transmitted to the temporomandibular joints (TMJ).
CONCLUSION
With proper planning and execution, odontectomy is normally safe and ends in predictable good prognosis. The incidence of any complications can be minimized by thorough preoperative assessment, radiographic assistance, adept surgical technique, and timely recognition of any adverse events that may occur.
Even if this procedure can be easily accomplished by most of experienced general dentists, DMD Center highly recommends that one should always create an informed consent to be signed by your patient prior to the surgery along with thorough discussion with him/her about all the possible risks of this procedure. By doing this, if in case complications do develop, the practitioner can readily address the situation, assess the possible alternative solutions and implement it with full cooperation of the patient.
Contributor:
Dr. Bryan Anduiza - Writer
Dr. Jean Villanueva - Editor
REFERENCES:
1. Baqain ZH, Al-Shafii A, Hamdan AA, Sawair FA. Flap design and mandibular third molar surgery: a split mouth randomized clinical study. Int J Oral Maxillofac Surg. 2012;41:1020–4. doi: 10.1016/j.ijom.2012.02.011
2. Marciani RD. Complications of third molar surgery and their management. Atlas Oral Maxillofac Surg Clin North Am. 2012;20:233–51. doi: 10.1016/j.cxom.2012.06.003.
3. Erdogan O, Tatlı U, Ustün Y, Damlar I. Influence of two different flap designs on the sequelae of mandibular third molar surgery. Oral MaxillofacSurg. 2011;15:147–52. doi: 10.1007/s10006-011-0268-7.
4. Sandhu A, Sandhu S, Kaur T. Comparison of two different flap designs in the surgical removal of bilateral impacted mandibular third molars. Int J Oral Maxillofacial Surg. 2010;39:1091–6. doi: 10.1016/j.ijom.2010.07.003.
5. Amin Rahpeyma, Saeedeh Khajehahmadi,* and Sina Ilkhani. Wound Dehiscence after Wisdom Tooth Removal in Mandibular Mesioangular Class IB Impactions: Triangular Transposition Flap versus Envelope Flap
6. Karaca I, Simşek S, Uğar D, BozkayaS BozkayaS. Review of flap design influence on the health of the periodontium after mandibular third molar surgery. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;104:18–23. doi: 10.1016/j.tripleo.2006.11.049.
7. Christiaens I, Reychler H. Complications after third molar extractions: retrospective analysis of 1,213 teeth. Rev Stomatol Chir Maxillofac. 2002;103:269–274.
8. Hupp JR, Ellis E, Tucker MR. Contemporary Oral and Maxillofacial Surgery. 6th ed. St. Louis: Mosby Elsevier; 2013.
9. Ghaeminia H, Meijer GJ, Soehardi A, Borstlap WA, Mulder J, Bergé SJ. Position of the impacted third molar in relation to the mandibular canal. Diagnostic accuracy of cone beam computed tomography compared with panoramic radiography. Int J Oral Maxillofac Surg. 2009;38:964–971.
10. Calvo AM, Brozoski DT, Giglio FP et al. Are antibiotics necessary after lower third molar removal? Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;114(5 Suppl):199–208.
11. Lang MS, Gonzales ML, Dodson TB. Do antibiotics decrease the risk of inflammatory complications after third molar removal in community practices? J Oral Maxillofac Surg.2017;75:249–255.
12. Sarna T, Sengupta T, Miloro M, Kolokythas A. Cervical necrotizing fasciitis with descending mediastinitis: literature review and case report. J Oral Maxillofac Surg. 2012;70:1342–1350.
13. Harada N, Vasudeva S, Joshi R, et al. Correlation between panoramic radiographic signs and high-risk anatomical factors for impacted mandibular third molars. Oral Surg. 2013;6:129–136.
14. McKenzie WS, Rosenberg M. Latrogenic subcutaneous emphysema of dental and surgical origin: a literature review. J Oral Maxillofac Surg. 2009;67:1265–1268.
15. Tarakji B, Saleh LA, Umair A, Azzeghaiby SN, Hanouneh S. Systemic review of dry socket: aetiology, treatment, and prevention. J Clin Diagn Res. 2015;9:10–13.
[dvk_social_sharing] [et_bloom_inline optin_id="optin_1"]