HOW DO YOU MANAGE AND TREAT YOUR PREGNANT PATIENTS?
Pregnancy is such a significant period of a woman's life wherein both hormonal and physiological changes can occur that may adversely affect her oral health. Pregnant women often do not seek dental care, as some of them believe that it is not safe for them to have certain dental procedures done. Preventive, diagnostic, and restorative dental treatment are safe throughout pregnancy and do improve ones oral health even during this delicate time. Here are some information you may need on how to manage our pregnant patients in our dental treatments:
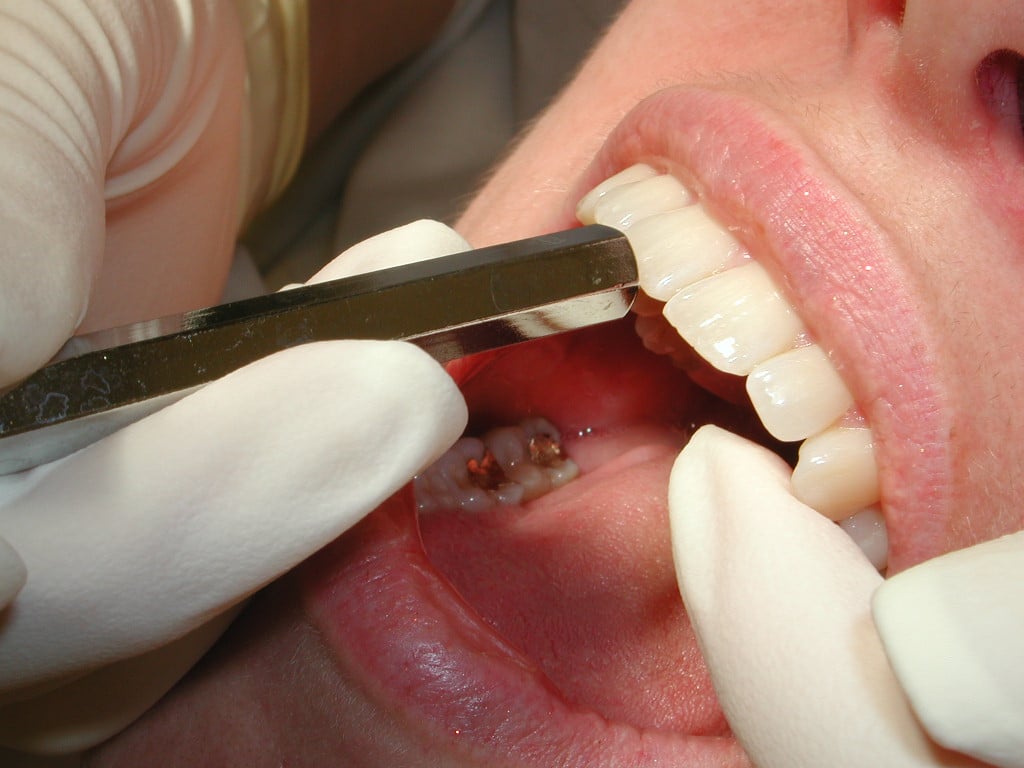
ORAL TOOTH EXTRACTION
During pregnancy, maintaining a good calcium level is a challenge, thus, this may result to our necessity to do extraction on a pregnant woman. So, can we do extraction during pregnancy?
Yes, however, oral extraction should be the last resort for us, dentists, to do on pregnant patients. In fact, oral extraction can actually be performed any time during pregnancy. However, as oral extraction is a form of surgery wherein we are required to do some steps or procedures that may not be acceptable for pregnant women, it is recommend that the ideal time to do so, if this dental treatment becomes necessary, is during the second trimester.
Moreover, it is important to take note that there is an increase of hormones during pregnancy such as the estrogen and progesteron hormones. Why? Because these two hormones act as an insulin antagonist which may lead to insulin resistance. As the body resists there's an automatic increase production of insulin to address the resistance being created by these hormones which may eventually lead to gestational diabetes. And, in oral extraction, we need our patients to have a good bleeding time and prognosis in healing after a surgical procedure. Thus, we should just provide palliative treatment instead of extraction unless emergency situation for pregnant women who are obese and/or with a positive family history of Type II diabetes mellitus. These pregnant women have a higher risk of developing gestational diabetes that can lead to further complcations during or after invasive dental procedure.
ANESTHETIC MANAGEMENT
It is very hard to identify which procedures and chemicals or substances that maybe harmful both for the mother and the baby inside as testing of such cannot easily be done as rarely pregnant women as subjects may not be viable nor scientists be willing to use them. Thus, we tend to side on the air of caution precisely because there's not much testing which is safe and not. So, what types of anesthetics are safe for pregnancy? The FDA (Food and Drug Administration has classified anesthetic in different categories to guide us, if the situation arises that we need to administer anesthetics due to dental procedure. They are the following:
I. NO EVIDENCE OF RISK IN HUMANS
CATEGORY A
- Adequate well-controlled studies in pregnant women have not shown increased risk of fetal abnormalities despite adverse findings in animals.
CATEGORY B
- In the absence of human studies, animal studies showed no fetal risk. The chance of fetal harm is remote but remains a possibility.
II. RISK CANNOT BE RULED OUT
CATEGORY C
- Adequate well-controlled human studies are lacking, and animal studies have shown a risk to the fetus or are lacking as well. There is a chance of fetal harm if administered during pregnancy, but the potential benefits may outweigh the potential risk. But, there might be positive evidence of risk.
III. POSITIVE EVIDENCE OF RISK
CATEGORY D
- Studies in humans, or investigational or post-marketing data, have demonstrated fetal risk. Nevertheless, potential benefits from use of this drug may outweigh the potential risk. For example, the drug may be acceptable if needed in a life-threatening situation or serious disease for which safer drugs cannot be used or are ineffective.
IV. CONTRAINDICATED TO PREGNANT WOMEN
CATEGORY X
- Studies in animals or humans, investigational or post-marketing reports, have demonstrated positive evidence of fetal abnormalities or risk that clearly outweighs any possible benefit to the patient.
Overall, in certain circumstances that anesthetic administration becomes necessary, it is still okay for us to use them. However, there are some considerations, including what type of anesthetic is used, how much is needed, and the stage of the pregnancy. Keep in mind that pregnancy does affect several organs, including the cardiovascular system, liver, and kidneys, and these may affect your body’s reaction to the anesthetic. Also, the anesthetic does go into the fetal circulation. This means it goes to the baby. During the first trimester, or 13 weeks of pregnancy, the baby’s organs and limbs are forming. It’s possible that the anesthetic could cause a birth defect. Considering this, it might be prudent to put off any elective procedure until after the pregnancy or later in the pregnancy.
It has been recommended that using Category A during the first trimester and during lactation with local anesthesia without vasoconstrictor to avoid possible idiosyncratic reaction to the fetus and neonate, not to the vasoconstrictor but to the preservative used to stabilize the vasoconstrictor. Category B anesthetics with vasoconstrictor is also safe to use for our pregnant patients. Under Category B with epinephrine, lidocaine is the safest. While under Category C, such as bupivacaine and mepivacaine maybe used but with caution. While those anesthetics containing felypressin should be avoided during pregnancy because this chemical constricts the blood vessels.
The following anesthetics are NOT recommended for pregnant women:
(a) Felypressin is a synthetic analogue of vasopressin. Vasopressin is a man-made form of a hormone called "anti-diuretic hormone" that is normally secreted by the pituitary gland. Vasopressin acts on the kidneys and blood vessels) with little of its antidiuretic or oxytocin-like actions. As such it may cause vasoconstriction and might affect the uterus during pregnancy.
(b) Prilocaine should not be used due to the risk of the fetus developing methemoglobinemia. In the second and third trimesters, proper positioning and heart rate monitoring are important to avoid postural hypotension.
(c) According to ADA studies, Nitrous Oxide is classified as a pregnancy risk group Category C medication, meaning that there is a risk of fetal harm if administered during pregnancy. It is recommended that pregnant women, both patients and staff, avoid exposure to nitrous oxide. The National Institute of Occupational Safety and Health (NIOSH), a US federal agency affiliated with the Centers for Disease Control and Prevention, recommends use of a scavenging system and exposure limits of N2O concentrations in dental operations to approximately 25 ppm during analgesia administration even to non-pregnant women or in general patients.
RADIOGRAPHIC ASSESSMENT MANAGEMENT
It is highly advisable that we avoid any radiographic examination during the first trimester as this is a very critical developmental stage of the fetus. So, if you need an x-ray done to assess the level of difficulty of the tooth you will extract, then, late 2nd and 3rd trimester will be good to do so, but, proper protective radiation management must be strictly observed. We should also opt to radiographic examination that does not require prolong exposure such a periapical x-ray as this very focus only on the area needed to be exposed and the radiation rays and time of exposure are very limited in comparison to other radiographic examinations like panoramic or CBCT scan.
PRESCRIPTION MANAGEMENT
Just like anesthetics, prescribing medicines are also categorized in the same manner, names and definitions by the US FDA as mentioned above. So, if you need to prescribed have a collaborative consult with the patient’s obstetrician to weigh risks and benefits. An example of a situation that may benefit from consultation is pain relief. Several analgesics have been placed in pregnancy Category B, which indicates that they are typically safe to use; however, in 2015, the U.S. Food & Drug Administration backed off that classification, stating that the published research is “too limited to make any recommendations” on pain reliever use in this population. This suggests that decisions made about medications for pain relief should be arrived at after consultation with the obstetrician. That said, emergencies call for immediate implementation of standard emergency protocols.
I. Suggested Medications under Category B
A. For Pain Relief
1. Acetaminophen
2. Paracetamol without caffeine
B. Antibiotics
1. Penicillin
2. Amoxicillin
3. Cephalosporins
4. Clindamycin
5. Metronidazole
Do take note that allergic test or history must be considered before prescribing these medicines.
II. Medications under Category C or X
A. For Pain Relief
1. Ibuprofen (Advil, Motrin)
High doses of this OTC pain reliever can cause many serious problems, including: miscarriage, delayed onset of labor, premature closing of the fetal ductus arteriosus, an important artery, jaundice, hemorrhaging for both mother and baby, necrotizing enterocolitis, or damage to the lining of the intestines, oligohydramnios, or low levels of amniotic fluid, fetal kernicterus (a type of brain damage), and abnormal vitamin K levels.
Most experts agree that ibuprofen is probably safe to use in small to moderate doses in early pregnancy. It’s especially important to avoid ibuprofen during the third trimester of pregnancy as studies show that it is during this stage of pregnancy that ibuprofen is more likely to cause heart defects on the baby.
2. Warfarin (Coumadin)
This is a blood thinner that’s used to treat blood clots as well as prevent them. It can cause birth defects. It should be avoided during pregnancy unless the risk of a blood clot is more dangerous than the risk of harm to the baby.
B. For Oral Hygiene
Mouth rinses are used as a daily regimen for dental hygiene. The active ingredients such as cetylpyridinium chloride, xylitol are generally safe, but, if the rinse contains alcohol, it should not be used by a pregnant woman. Even though the individual spits out most of the rinse, there is as much as 9%-14% of alcohol that can still be swallowed or absorbed by the patient.
C. For Antibiotics
1. Ciprofloxacin (Cipro) and Levofloxacin
These are a types of antibiotics. These drugs could cause problems with the baby’s muscle and skeletal growth as well as joint pain and potential nerve damage in the mother. Ciprofloxacin and Levofloxacin are both Fluoroquinolone antibiotics. Fluoroquinolones can increase the risk of aortic tears or ruptures. This can result in life-threatening bleeding. People with a history of aneurysms or certain heart diseases may be at an increased risk of side effects. Fluoroquinolones also increase the chances of having a miscarriage, according to a 2017 study.
2. Tetracycline
Tetracycline such as tetracycline, minocycline and doxycycline are types of broad spectrum antibiotic that should not be suggested at any time during pregnancy. As it may cause permanent yellow-gray-brown discoloration of the teeth and enamel hypoplasia to the baby. The use of tetracycline during pregnancy is generally not recommended, especially during the last half of pregnancy.
CONCLUSION
In conclusion, it is very important that as their dentists we are abreast with the right knowledge and proper protocols to manage this type of patients. This is a very sensitive and important time of their lives, thus, we have to be sure that as we do our dental treatments to handle their oral health concerns that we also protect the safety of both the mother and baby in her womb. A collaborative consult with her obstetrician is a must especially in elective dental procedures and providing the patient herself the correct information on pre and post op oral care instruction with full understanding on her part. Let's share this happy period on our patient's life by providing them excellent dental care during this time that they can appreciate.
Contributors:
Dr. Jean Galindez - Writer | Main Editor
Dr. Bryan Anduiza - Writer
References:
1. Jacobsson B, Kacerovsky M, Menon R, Musilova I, Radochova V, Slezak R, Stepan M, Vescicik P (2019) ‘Association between periodontal disease and preterm prebalor rupture of membranes'. Journal of Clinical Periodontology
2. Sacdev R, Garg K (2015) ‘ Review on pregnancy and Oral health: A question to care’ . Indian Journal applied research