HOW DO WE DEAL WITH COVID-19?
Before we deal with CoVid-19 virus, let's deal first in general the 3 critical factors as to how experts, medical professionals, virologists and scientists deal with handling viruses that can result to preventing and containing communicable diseases:
1. The experts need to fully know through factual data and studies about the genetics, mutations and other relevant information about the virus causing the disease.
2. The experts through #1 are able to develop vaccine that can prevent it and if humans are infected, its treatment to address it.
3. The human factor and its social behaviors that can prevent, contain and totally eliminate this virus that can result to an epidemic or pandemic and become detrimental to human beings.
So, knowing these 3 critical factors, only #3 when it comes to CoVid-19 virus is the only one we have in full control, as of the moment, to arm ourselves to contain this from its continuous onslaught to our global society.
CORONAVIRUS FAMILY
Coronaviruses family have been in existence for quite some time now. This a group of viruses that have a halo or crown-like (corona) appearance when viewed under a microscope. They are considered to be zoonotic, meaning they are transmitted between animals and people. This virus has mutated into various forms and categorized as a large family group of virus that majorly affects the respiratory system. This family of virus can cause health issues ranging from common colds to the most severe ones such as 2 of the previously known viruses that created these communicable diseases:
1. Middle East Respiratory Syndrome (MERS-CoV) occured in 2012 wherein majority of the cases are found in Saudi Arabia and transmitted from dromedary camels to humans. It is believed that this originated from bats and then, transferred to camels. This is probably why there is a circulating assumption from CDC that CoVid-19 virus originated from bats as well, but, currently, there's simply no concrete evidence yet that it is. MERS-CoV base on laboratory studies has a higher mortality rate of approximately 35% which is not the case on CoVid-19 base on real time data. The percent of human to human transmission is quite low on MERS-CoV virus as it does not pass easily human to human unless there is close contact, such as providing unprotected care to an infected patient, especially when infection prevention and control practices are inadequate or inappropriate. This is not the case of CoVid-19 as human to human transmission is quite high and fast.
2. Severe Acute Respiratory Syndrome (SARS-CoV) became an epidemic in 2003, after first appearing in Southern China in November 2002 and was transmitted from civet cats to humans. The SARS-CoV appears to spread by close person-to-person contact, transmitted most readily by respiratory droplets (droplet spread) produced when an infected person coughs or sneezes. Droplet spread can happen when droplets from the cough or sneeze of an infected person are propelled a short distance (generally up to 3 feet) through the air and deposited on the mucous membranes of the mouth, nose, or eyes of persons who are nearby. The virus also can spread when a person touches a surface or object contaminated with infectious droplets and then touches his or her mouth, nose, or eye(s). In addition, it is possible that SARS-CoV might be spread more broadly through the air (airborne spread) or by other ways that are not now known. This has a mortality rate of 9.6%.
Sounds familiar? This is probably the reason why the Chinese doctors, Dr. Li Wenliang, the medical doctor who first initiated an alarm about CoVid-19 thought that the increasing number of cases he was seeing in his practice is SARS.
FACTS on CoVid-19
Like any family, CoVid-19 is similar but not exactly the same as the rest of its coronavirus family. Thus, WHO globally extrapolate all data in regards to CoVid-19 that's mostly derived from the information provided by China's Center for Disease Control, from references on the general studies and records of its relative coronaviruses mentioned above done by experts, and, the initial current cases seen and observed from other countries with high cases of CoVid-19.
So, what exactly are we dealing with? Here are already undisputed facts:
- It is also known as 2019 novel coronavirus.
- The virus name is SARS-CoV-2 virus, a betacoronavirus just like MERS and SARS.
- The first report of this virus occurred at Wuhan, Hubei Province, China in December 2019 and had some link to a large seafood and live animal market, suggesting animal-to-person spread.
- Common signs of infection include respiratory symptoms, fever, cough, shortness of breath and breathing difficulties. In more severe cases, infection can cause pneumonia, severe acute respiratory syndrome, kidney failure and even death.
- Just like SARS-CoV, it is mainly transmitted through contact with respiratory droplets rather than through the air. The disease can spread from person to person through small droplets from the nose or mouth which are spread when a person with COVID-19 coughs or exhales. These droplets land on objects and surfaces around the person. Other people then catch COVID-19 by touching these objects or surfaces, then touching their eyes, nose or mouth. People can also catch COVID-19 if they breathe in droplets from a person with COVID-19 who coughs out or exhales droplets. This is why it is important to stay more than 1 meter (3 feet) away from a person who is sick.
- The median incubation period is five to seven days, with the longest incubation period as 14 days.
- This is now considered by WHO as a pandemic.
- The test kit used to detect this virus is called real-time RT (reverse transcription)-polymerase chain reaction (rRT-PCR) detection of the SARS-CoV-2 virus (the virus that causes COVID-19) in respiratory specimens. It typically involves taking a swab from deep in a patient's nasal cavity to collect cells from the back of the nose. Test can be virtually done anywhere and it takes 24-72 hours to get the results of the test. There's an estimated 3 results released that contain errors because even if acquiring the specimens from suspected CoVid-19 patients are easier, the process that the testing goes through from RNA to DNA sequencing is quite complicated. Although, CDC is developing a serology test to make testing more accurate.
So, what are basic information that can be considered factual as of the moment but can still change or vary depending on the further development and data provided by all countries affected by this:
1. How easily a virus spreads from person-to-person and if the spread is sustainable wherein it can spread continually without stopping?
- The virus that causes COVID-19 seems to be spreading easily and sustainably in the community (“community spread”) in some affected geographic areas. Community spread means people have been infected with the virus in an area, including some who are not sure how or where they became infected.
- It is not certain how long the virus that causes COVID-19 survives on surfaces, but it seems to behave like other coronaviruses. Studies suggest that coronaviruses (including preliminary information on the COVID-19 virus) may persist on surfaces for a few hours or up to several days. This may vary under different conditions (e.g. type of surface, temperature or humidity of the environment).
- The likelihood of an infected person contaminating commercial goods is low and the risk of catching the virus that causes COVID-19 from a package that has been moved, travelled, and exposed to different conditions and temperature is also low.
- Studies to date suggest that the virus that causes COVID-19 is mainly transmitted through contact with respiratory droplets rather than through the air.
- The risk of catching COVID-19 from someone with no symptoms at all is very low. However, many people with COVID-19 experience only mild symptoms. This is particularly true at the early stages of the disease. It is therefore possible to catch COVID-19 from someone who has, for example, just a mild cough and does not feel ill.
- The risk of catching COVID-19 from the feces of an infected person appears to be low. While initial investigations suggest the virus may be present in feces in some cases, spread through this route is not a main feature of the outbreak.
2. How virulent and deadly is CoVid-19?
- China say preliminary research shows that COVID-19 is mutating and there are at least two types of the virus now. Scientists dubbed the aggressive strain “L type” and the less prevalent version “S type.” The L type strain was seen more frequently in Wuhan, where the outbreak began, but researchers note that the frequency of infection has dropped off. They also cautioned that the data they had available for study was “very limited” and follow-ups were necessary to understand the evolution of the COVID-19.
- The complete clinical picture with regard to COVID-19 is not fully known. Reported illnesses have ranged from very mild (including some with no reported symptoms) to severe, including illness resulting in death. While information so far suggests that most COVID-19 illness is mild, a report out of China suggests serious illness occurs in 16% of cases. Older people and people of all ages with severe underlying health conditions — like heart disease, lung disease and diabetes, for example — seem to be at higher risk of developing serious COVID-19 illness.
- COVID-19 outbreaks can be contained and transmission stopped, as has been shown in China and some other countries.
- The risk depends on where you are - and more specifically, whether there is a COVID-19 outbreak unfolding there. For most people in most locations the risk of catching COVID-19 is still low. However, there are now places around the world (cities or areas) where the disease is spreading. For people living in, or visiting, these areas the risk of catching COVID-19 is higher.
- Illness due to COVID-19 infection is generally mild, especially for children and young adults. However, it can cause serious illness: about 1 in every 5 people who catch it need hospital care.
- According to the data provided by China, more than 72,000 COVID-19 cases reported in mainland China reveals a case-fatality rate (CFR) of 2.3% and suggest most cases are mild, but the CFR jumped considerably among older patients, to 14.8% in patients 80 and older, and 8.0% in patients ages 70 to 79.
- While there has been one instance of a dog being infected in Hong Kong, to date, there is no evidence that a dog, cat or any pet can transmit COVID-19. COVID-19 is mainly spread through droplets produced when an infected person coughs, sneezes, or speaks.
INFECTION CONTROL MANAGEMENT
It goes without saying that with or without CoVid-19 virus, as health providers and professionals, plus, hopefully, a decent human being with conscience, we always practice infection control protocols in our dental practice. Doing the proper infection control protocol will never be cheaper, convenient and an option. It is a must and we should never compromise on things that truly matters as this protocol is first and foremost for your protection and not your patients. We are the most vulnerable on communicable and dangerous diseases as we are fully exposed to the most common mode of transmission of these diseases, just like CoVid-19. We also need to understand the main function and purpose of these protective gears that WHO and the Centers for Disease Control and Prevention have listed for health workers like us should do to prevent us from being infected and/or a carrier of these viruses. Remember, virus, bacteria and other microorganisms are not discriminatory of whom it would like to affect and our excuses whether justifiable or not, will not matter to it. CoVid-19 and other even more dangerous and contagious diseases will not care if face masks is out of stock or autoclave is expensive or medical grade disinfectants are difficult to acquire, etc. Moreover, if you don't care about your health and willing to die any time, what about your love ones, your co-workers, and your patients who are even paying you for them just to acquire a disease or even die because we want to compromise and justify our excuses even if it is not right? As I've always mentioned in my lectures, the practice of dentistry is always the practice of our conscience whether on this issue or in our choice of doing our dental treatments.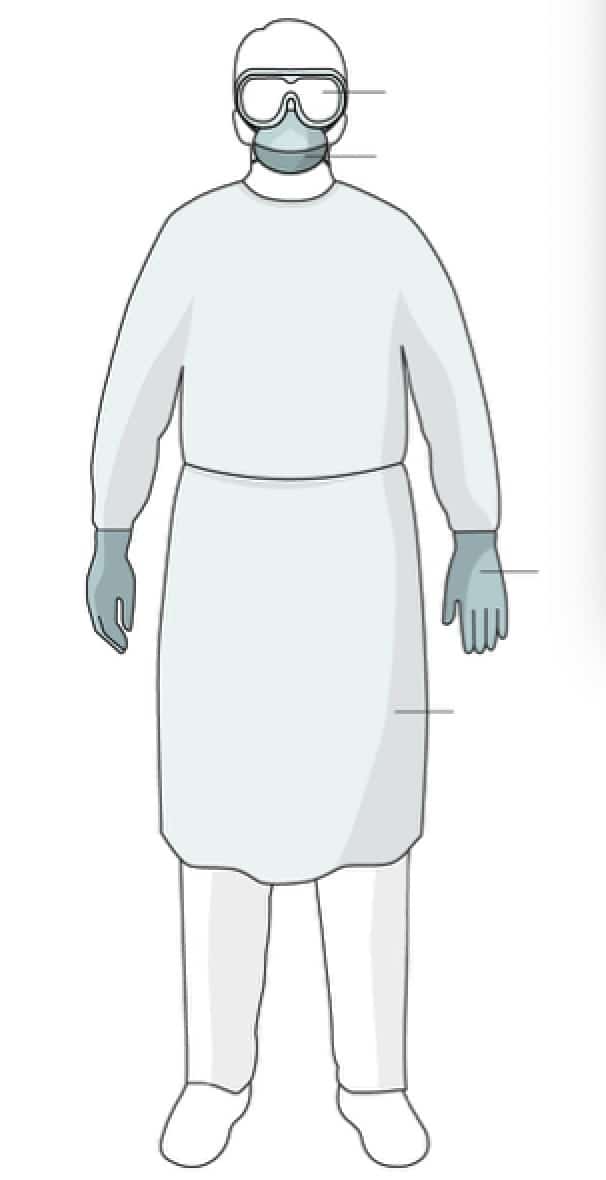
- Eye Protection – Goggles or Face Shield - Our eyes is one of our organs that makes us truly vulnerable in communicable diseases especially if we are doing surgical procedures. For example, in HIV virus, if the blood of our patient that's HIV + goes into our eyes, almost 100% you'll acquire AIDS. The same as CoVid-19.
- Respirator or Face Mask – It seems there's a misconception of many professionals why they wear a face mask. Face mask is NOT just to cover your face but, first and foremost to filter the virus and bacteria that you will mostly inhale or absorbed by your skin. Thus, the type of face mask you will use depends on what type of procedure you are doing or what your are protecting yourself with. Your procedural masks will never protect you and when it states "disposable", it is disposable, there's no ifs and buts on it. It means for single use only. For dentists, BFE (Bacterial Filtration Efficiency) base on ASTM (American Society of Testing and Materials), the standard must be at least a minimum 95% filtration for non-surgical procedures and PFE (Particulate Filtration Efficiency) must be particle size of 0.1 micro. When a disposable face mask gets wet or the Fluid Resistance of the face mask used is low, then, automatically, that face mask is rendered useless for any protection. This is the reason why in highly contagious diseases a N95 face mask is generally recommended.
Strict guidelines of WHO for Face Mask if you want to Protect Yourself from CoVid-19:
(a) Before putting on a mask, clean hands with alcohol-based hand rub or soap and water.
(b) Cover mouth and nose with mask and make sure there are no gaps between your face and the mask.
(c) Avoid touching the mask while using it; if you do, clean your hands with alcohol-based hand rub or soap and water.
(d) Replace the mask with a new one as soon as it is damp and do not re-use single-use masks.
(e) To remove the mask: remove it from behind (do not touch the front of mask); discard immediately in a closed bin; clean hands with alcohol-based hand rub or soap and water.
According to WHO: "The following measures ARE NOT effective against COVID-2019 and can be harmful:"
- Smoking
- Wearing multiple masks
- Taking antibiotics
- Gloves – fitted above the wrist
- Gown – closed securely at the back
Here are Some General Tips for Dental Practitioners Inside the Clinic:
- Dentists should take strict personal protection measures and avoid or minimize operations that can produce droplets or aerosols.
- The 4-handed technique is beneficial for controlling infection.
- Make sure that the saliva ejectors and high volume evacuation tips are working well as this can reduce the production of droplets and aerosols.
- Clinicians must wash their hands thoroughly for at least 20 seconds every after procedure.
- If water and soap is not available, use a hand sanitizer which contains at least 60% alcohol.
- Avoid touching nose, eyes, face, mouth with unwashed hands.
- Avoid close contact with sick people
- Disinfect your dental chair, tables, light handles, handpieces and chairs after use
- If possible, use a eye shield to avoid spread of droplets in the face
- Stay home when you are sick.
- Avoid public places if necessary.
- Cover your cough or sneeze with a tissue, throw the tissue in the trash, and then wash your hands.
- Clean and disinfect frequently touched objects and surfaces
- Sick employees shouldn't return to work until their temperature has stayed below 37.8 degrees Celsius for at least 24 hours, without the help of fever-reducing or other symptom-altering medicine.
- Provide disposable wipes so that commonly used surfaces (for example, doorknobs, keyboards, remote controls, desks) can be wiped down by employees before each use
- Disinfect and sterilized properly all your dental instruments and materials that are NOT disposable.
Tips on Evaluation of Patients:
- During the outbreak of the virus, establish a pre-check triages to measure and record the temperature of every staff and patient as a routine procedure. Asks patients questions about the health status and history of contact or travel.
- Patients and their accompanying persons are provided with medical masks and temperature measurement once they enter the hospital.
- Patients with fever should be registered and referred to designated hospitals. If a patient has been to epidemic regions within the past 14 days, re-schedule the treatment and advice patient to have a self-quarantine for at least 14 days and if becomes symptomatic to call their medical doctor.
Tips on Oral Examination:
- Preoperative antimicrobial mouth rinse could reduce the number of microbes in the oral cavity.
- Procedures that are likely to induce coughing should be avoided. Position the dental chair during treatment that will prevent the patient undue urge of coughing due water and debris streaming to their throat.
- Aerosol-generating procedures, such as the use of a 3-way syringe, should be minimized as much as possible.
- Intraoral x-ray examination can stimulate saliva secretion and coughing. Therefore, extraoral dental examinations, such as panoramic radiography and cone beam CT, are appropriate alternatives during the outbreak of COVID-19.
Tips on Treatment for Emergency Cases:
- Rubber dams and high-volume saliva ejectors can help minimize aerosol
- Face shields and goggles are essential with use of high- or low-speed drilling with water spray
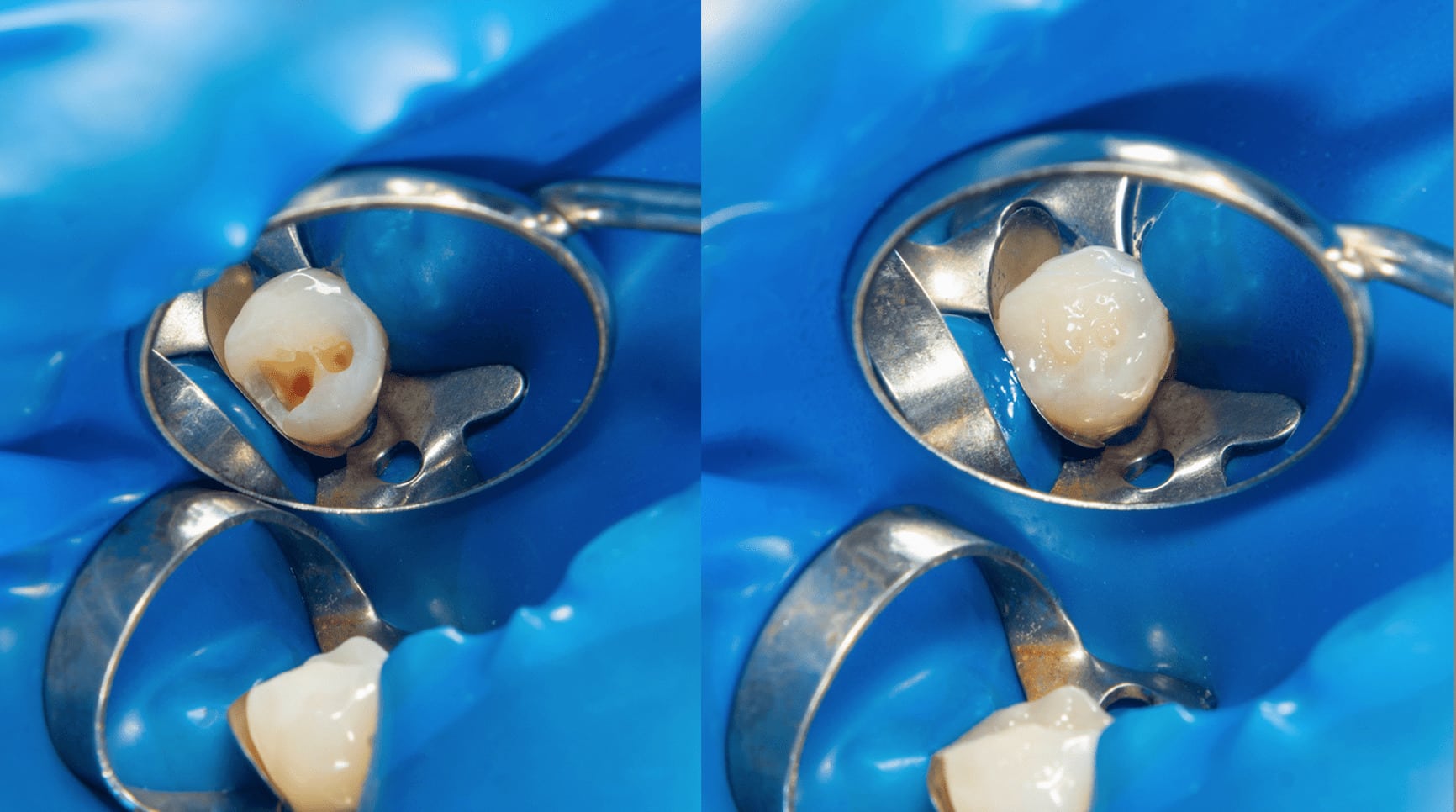
- If a carious tooth is diagnosed with symptomatic irreversible pulpitis, pulp exposure could be treated with chemo-mechanical caries removal under rubber dam isolation and a high-volume saliva ejector after local anesthesia; Pulp devitalization can be performed to reduce the pain.
- After treatment, environmental cleaning and disinfection procedures is a necessity. Alternatively, patients could be treated in an isolated and well-ventilated room.
- If a tooth needs to be extracted, absorbable suture is preferred. For patients with facial soft tissue contusion, debridement and suturing should be performed. It is recommended to cover with wrapped cotton with gauzed as we rinse the wound slowly and use the saliva ejector to avoid spraying.
CONCLUSION
In conclusion, in order to fight something we don't see and can't fully control we have to arm ourselves with facts. I always say "Knowledge is Power", this is even more apparent and needed on our current situation. We have to know real facts, "evidence base" as I hear from our dental community more often than I care about (the reason why is irrelevant on this post), but, on this case, "evidence base" facts are truly important, in fact, non-negotiable. Thus, knowing facts with basis will allow us to act and react properly to contain and combat this virus that's creating havoc globally and be part of the solution rather than additional problem.
Contributors:
Dr. Jean Galindez - Writer | Main Editor
Dr. Bryan Anduiza - Writer
References:
WHO (World Health Organization) Website - https://www.who.int
CDC Website - https://www.cdc.gov